Background
Attention-deficit/hyperactivity disorder (ADHD) is a common diagnosis in childhood, characterized by persistent impairing inattention, hyperactivity, and impulsivity with symptoms recognized in patients before age 12.1 Since ADHD is the most common pediatric neurodevelopmental disorder diagnosed in the U.S., this condition has readiness and force health importance to the Department of Defense (DOD), and its high prevalence in the adolescent and adult civilian population affects the pool of military applicants.2 Current DOD accession policy lists ADHD as disqualifying for military applicants if they meet any of the following conditions: ADHD medication prescribed in the previous 24 months, an educational plan or work accommodation after age 14, a history of comorbid mental health disorders, or documentation of adverse academic, occupational, or work performance.3
The prevalence of ADHD in U.S. children aged 2–17 is estimated to range from 9–11% with approximately two-thirds of children with ADHD having at least 1 other mental, emotional, or behavioral disorder.4 In 2016, U.S. surveillance data revealed that 62% of children diagnosed with ADHD currently take medication for the condition.5 Although symptoms can resolve after childhood, the most recent estimate of overall prevalence of adult ADHD in the U.S. is 4.4%.4 Unpublished data from an analysis conducted using Defense Medical Surveillance System (DMSS) data, demonstrated annual ADHD prevalence estimates ranging from 1.7–3.7% in the active component from 2000–2016 with a peak prevalence in 2011 (E. T. Reeves, MD, unpublished data, 2017). Although patients with ADHD are more likely to have comorbid mood, anxiety, and substance use disorders,4,6–8 patients receiving ADHD medications may be protected from the development of these associated mental health conditions.9,10
The last major change to DOD accession policy standards for ADHD occurred in 2010 and resulted in more restrictive requirements (no medications for more than 24 months cumulative after age 14 instead of the previous requirement of no medications within 12 months of enlistment). Although services can accept applicant waivers with less stringent restrictions (e.g., the Air Force will consider waivers for recruits stable off medications for 15 months), ADHD diagnosis is consistently a common disqualifier for military service. In 2017, ADHD and disruptive behavior disorders were the fifth most frequent medical disqualification of first-time enlisted active component military applicants.11 Although previous studies have evaluated the impact of ADHD on retention rates2 (also E. T. Reeves, MD, unpublished data, 2017) and its association with post-traumatic stress disorder (PTSD),6,8 no surveillance data have been published on recent estimates of the prevalence of ADHD diagnoses in active component military personnel or on what proportion of active component service members with ADHD are dispensed ADHD medications. The primary objectives of this study were to determine the prevalence of ADHD diagnoses among active component service members from 2014 through 2018 and the proportion of these service members who were prescribed medications to treat the condition.
Methods
This descriptive study utilized a surveillance period from 1 January 2014 through 31 December 2018. The surveillance population included any member of the Army, Navy, Air Force, or Marine Corps who served in the active component at any point during the surveillance period. All data used to identify prevalent cases of ADHD were derived from records routinely stored in the DMSS, which is maintained by the Armed Forces Health Surveillance Division (AFHSD). DMSS includes medical encounter data (e.g., outpatient visits, hospitalizations) of active component members of the U.S. Armed Forces in military and civilian (if reimbursed through the Military Health System) treatment facilities. The DMSS also includes medical screening data from Military Entrance Processing Stations (MEPS) and records of prescribed and dispensed medications from the Pharmacy Data Transaction Service (PDTS) which were also included in this analysis.
For surveillance purposes, an ADHD case was defined as a qualifying ADHD diagnosis in the first or second diagnostic position for diagnoses assigned during MEPS medical screening; or 1 hospitalization with any of the qualifying diagnoses of ADHD in the first or second diagnostic position; or 2 outpatient medical encounters within 180 days of each other, with any of the defining diagnoses of ADHD in the first or second diagnostic position; or 1 outpatient/TMDS medical encounter in a psychiatric or mental health specialty care setting, identified by a Medical Expense and Performance Reporting System (MEPRS) code beginning with 'BF', with a qualifying diagnosis of ADHD in the first or second diagnostic position. The International Classification of Diseases, 9th Revision (ICD-9) and International Classification of Diseases, 10th Revision (ICD-10) codes used to identify ADHD cases included all those falling under the parent codes 314 and F90, respectively.
Individuals with a diagnosis of ADHD at any time during the surveillance period were assumed to be prevalent cases at the time of accession regardless of when they were formally diagnosed, since the Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM-5) requires the presence of symptoms prior to age 12 to meet the diagnostic criteria for ADHD.1
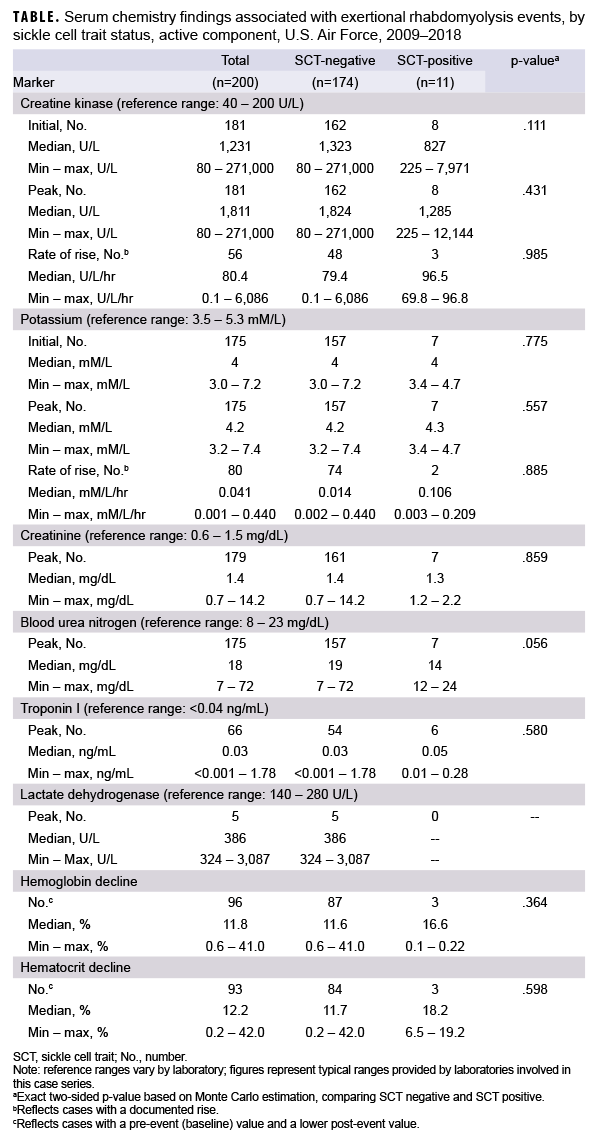
To qualify as treated for ADHD, service members had to have a PDTS record documenting that they had been dispensed an FDA-licensed drug for the treatment of ADHD at least twice within 6 months (181 days) which is consistent with previous research.10 Active component service members dispensed ADHD medication with longer gaps than this threshold were classified as untreated. Medications used for the treatment of ADHD included stimulants (amphetamines, methylphenidates), guanfacine (Intuniv), clonidine (Kapvay), and atomoxetine (Strattera). Table 1 presents a comprehensive list of ADHD medications used in the current analysis.
Crude annual prevalence of ADHD in the active component of the military during 2014–2018 were calculated and reported as percentages. In these calculations, the numerator was the number of prevalent cases of ADHD in active component service members and the denominator included all active component service members in service as of 30 June in the specified year. The proportion of active component service members diagnosed with ADHD who had been dispensed ADHD medication as defined above was calculated. Service members for whom ADHD medication was dispensed (treated) and those for whom ADHD medication was not dispensed (untreated) were compared on several background variables (i.e., sex, age group, race/ethnicity group, education level, marital status, branch of service, rank/grade, and military occupation) using chi-square tests. All analyses were conducted using SAS/STAT software, version 9.4 (2014, SAS Institute, Cary, NC).
Results
During the 5-year surveillance period, the crude annual ADHD prevalence among the active component declined from 3.9% in 2014 (n=58,691) to 2.8% in 2018 (n=41,338) (Figure 1). Compared to their respective counterparts, service members with less than a high school education, those who were divorced or widowed, non-Hispanic whites, Army members, senior enlisted members, and those in healthcare occupations had higher overall prevalence rates of ADHD. Females and males had similar annual and overall prevalence estimates (Figure 2, Table 2). Junior enlisted (E1–E4) service members trended down from the group with the second highest prevalence in 2014 to the group with the lowest prevalence in 2018 (Table 2, Figure 3).
The proportion of prevalent ADHD cases who were prescribed ADHD medication during the surveillance period was 60.2%. During the surveillance period, the majority of medications prescribed were stimulants alone (78.9–79.6%) compared to combined stimulant and non-stimulant (16.5–17.4%) or non-stimulant only (3.6%–3.9%) regimens (Figure 4). ADHD patients were more likely to be dispensed medication if they were older than 25 years of age, above junior enlisted rank (E1–E4), divorced/widowed, or in a healthcare occupation (Table 3).
Editorial Comment
This report documents the prevalence and medication trends of ADHD among the active component service members during 2014–2018. Previous unpublished data on crude annual ADHD prevalence in the active component prior to 2014 revealed that a peak prevalence occurred in 2011 (E. T. Reeves, MD, unpublished data, 2017). The current study demonstrated a continued decline in the crude annual prevalence of ADHD in the military since the ADHD accession medical standard became more restrictive in 2010, particularly among junior enlisted (E1–E4) service members whose crude annual ADHD prevalence was lower than all other rank groups in 2018. In contrast, national adult ADHD prevalence rose during this same timeframe.12 The current study demonstrated a continued decline in the crude annual prevalence of ADHD in the military since the ADHD accession medical standard became more restrictive in 2010, particularly among junior enlisted (E1–E4) service members whose crude annual ADHD prevalence was lower than all other rank groups in 2018. In contrast, national adult ADHD prevalence rose during this same timeframe.12
The ADHD population in the DOD differs from that in the U.S. civilian population on several key demographic characteristics. Female and male service members have similar prevalences whereas adult males are approximately twice as likely to be diagnosed with ADHD compared to females in the U.S. civilian population.4,5,13 Possible explanations for this finding include that the true ADHD prevalence in males and females may be more similar than previous research has suggested when performing comparable occupations or indicates that males with ADHD may have characteristics (such as more recent medication use) selecting them to be disqualified from the military enlistment process at higher rates than females. Additionally, annual ADHD prevalences among service members in healthcare occupations were consistently more than 2 times the prevalences of those in other occupations. The reasons for this difference are unknown but may reflect better access to care, more knowledge about ADHD and treatment options, greater acceptance by coworkers, and/or less physical exertion-based/more sedentary jobs compared to other military occupations.
Medication dispensed for ADHD in the military (60%) represents a proportion similar to that in the U.S. civilian population (62%).4,14 These data and the distribution of medication for ADHD patients should be informative for commanders and providers. For example, stimulant medication, as a controlled substance, can only be prescribed for 3 months at a time, which complicates the deployment readiness of service members with ADHD.
Several limitations should be considered when interpreting the results of this study. The current study used data on medications dispensed to active component service members through PDTS, but the medication adherence of these patients could not be assessed. Furthermore, patients with ADHD in this study could have been prescribed the medications for other medical conditions (FDA approved indications or off-label use) or have obtained medications by other means without a prescription. Observational studies are subject to bias. For example, the (e.g., more severe symptoms or comorbid diseases) from the population of ADHD patients without medication. Diagnostic data were derived from coded medical encounters, including medical examination at MEPS, according to standardized health surveillance case definitions; however, this method may underestimate the prevalence of ADHD, especially in service members not actively being treated with medication for ADHD or who were deliberately withholding information related to prior ADHD diagnosis at MEPS assessment (i.e., misclassification bias). The earliest year of data collection was 2014 because of the inability to link to pharmacy data prior to that year.
In conclusion, this study found a decreasing trend in crude annual ADHD prevalence in the active component from 2014–2018. In terms of military readiness, a decrease in prevalence lessens the demand on commanders and medical practitioners to make decisions about whether or not ADHD is a waiverable condition for deployments; however, this must be balanced with the effects that a strict ADHD accession policy has on limiting the pool of military applicants. Continued research and discussions should focus on the optimal ADHD accession military standard. Future studies should evaluate the impact of deployment on ADHD patients, the high prevalence of ADHD in healthcare occupations, and differences among service members with ADHD accessed to the military through various methods (i.e., MEPS, waivers, withholding the diagnosis, new ADHD diagnosis).
Author Affiliations: Department of Preventive Medicine and Biostatistics, Uniformed Services University of the Health Sciences, Bethesda, Maryland (Maj Sayers); Defense Health Agency, Armed Forces Health Surveillance Division (Ms. Zhu, Dr. Clark).
Disclaimer: The views expressed herein are those of the authors and do not necessarily reflect official policy or position of Uniformed Services University of the Health Sciences, the Department of Defense, or Departments of the Army, Navy, or Air Force.
References
- American Psychiatric Association. Attention deficit and disruptive behavior disorders. In: Diagnostic and Statistical Manual of Mental Disorders. 5th ed (DSM-5). Arlington, VA: American Psychiatric Association; 2013.
- Krauss MR, Russell RK, Powers TE, Li L. Accession standards for attention-deficit/hyperactivity disorder: a survival analysis of military recruits, 1995–2000. Mil Med. 2006;171(2):99-102.
- Office of the Under Secretary of Defense for Personnel and Readiness. Department of Defense Instruction 6130.03. Medical Standards for Appointment, Enlistment, or Induction in the Military Services. 6 May 2018.
- Centers for Disease Control and Prevention. Data and Statistics About ADHD. https://www.cdc.gov/ncbddd/adhd/data.html. Accessed 5 September 2019.
- Danielson ML, Bitsko RH, Ghandour RM, Holbrook JR, Kogan MD, Blumberg SJ. Prevalence of parent-reported ADHD diagnosis and associated treatment among US children and adolescents, 2016. J Clin Child Adolesc Psychol.2018;47(2):199–212.
- Howlett JR, Campbell-Sills L, Jain S, et al. Attention deficit hyperactivity disorder and risk of posttraumatic stress and related disorders: A prospective longitudinal evaluation in US Army soldiers. J Trauma Stress. 2018;31(6):909–918.
- Spencer AE, Faraone SV, Bogucki OE, et al. Examining the association between posttraumatic stress disorder and attention-deficit/hyperactivity disorder: a systematic review and meta-analysis. J Clin Psychiatry. 2016;77(1):72–83.
- Ivanov I, Yehuda R. Optimizing fitness for duty and post-combat clinical services for military personnel and combat veterans with ADHD—a systematic review of the current literature. Europ J Psychotraumatol.2014;5(1):23894.
- Biederman J, DiSalvo M, Fried R, Woodworth KY, Biederman I, Faraone SV. Quantifying the protective effects of stimulants on functional outcomes in attention-deficit/hyperactivity disorder: A focus on number needed to treat statistic and sex effects. J Adolesc Health. 2019;65(6):784–789.
- Chang Z, D’Onofrio BM, Quinn PD, Lichtenstein P, Larsson H. Medication for attention-deficit/hyperactivity disorder and risk for depression: a nationwide longitudinal cohort study. Biol Psychiatry. 2016;80(12):916–922.
- Department of Defense. Accession Medical Standards Analysis and Research Activity Annual Report 2018. Silver Spring, MD: Statistics and Epidemiology Branch, Walter Reed Army Institute of Research; 2018.
- Chung W, Jiang S-F, Paksarian D, et al. Trends in the prevalence and incidence of attention-deficit/hyperactivity disorder among adults and children of different racial and ethnic groups. JAMA NetwOpen. 2019;2(11):e1914344.
- Kessler RC, Adler L, Barkley R, et al. The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. Am J Psychiatry. 2006;163(4):716–723.
- Danielson ML, Visser SN, Chronis-Tuscano A, DuPaul GJ. A national description of treatment among United States children and adolescents with attention-deficit/hyperactivity disorder. J Pediatr. 2018;192:240–246.e1.