What are the new findings?
In 2021, the overall numbers and rates of active component service member ambulatory care visits were the highest of any of the last 10 years. Most categories of illness and injury showed modest increases in numbers and rates. The proportions of ambulatory care visits that were accomplished via telehealth encounters fell to under 15% in 2021, compared to 19% in 2020.
What is the impact on readiness and force health protection?
Although the response to the COVID-19 pandemic in 2020 may have been associated with decreases in the incidence of disease and injury diagnoses in the service member population receiving ambulatory care, the data for 2021 show a return to pre-pandemic levels. Moreover, the proportions of health care encounters delivered through telehealth have similarly reverted to the lower levels seen in the pre-pandemic period. Lessons learned may guide future steps in reducing disease and injury incidence in the postpandemic era.
This report documents the frequencies, rates, trends, and characteristics of ambulatory healthcare visits of active component members of the U.S. Army, Navy, Air Force, and Marine Corps during 2021. Ambulatory visits of U.S. service members in fixed military and nonmilitary (reimbursed through the Military Health System [MHS]) medical treatment facilities are documented with standardized records that are routinely archived for health surveillance purposes in the Defense Medical Surveillance System (DMSS). Ambulatory visits that are not routinely and completely documented within fixed military and non-military medical treatment facilities (e.g., during deployments, field training exercises, or at sea) are not included in this analysis.
As in previous MSMR reports, all records of ambulatory visits of active component service members were categorized according to the International Classification of Diseases, 10th Revision (ICD-10) codes entered in the primary (first-listed) diagnostic position of the visit records.1 In this analysis, a special query of the DMSS records was performed to distinguish ambulatory visits that were accomplished via “telehealth” encounters (e.g., via telephone or video teleconference) rather than in-person encounters. Both types of encounters were included and not distinguished in most of the data summaries, but trends in the proportions of encounters that were accomplished via telehealth were examined because of the increased use of telehealth encounters during the COVID-19 pandemic.
Frequencies, rates, and trends
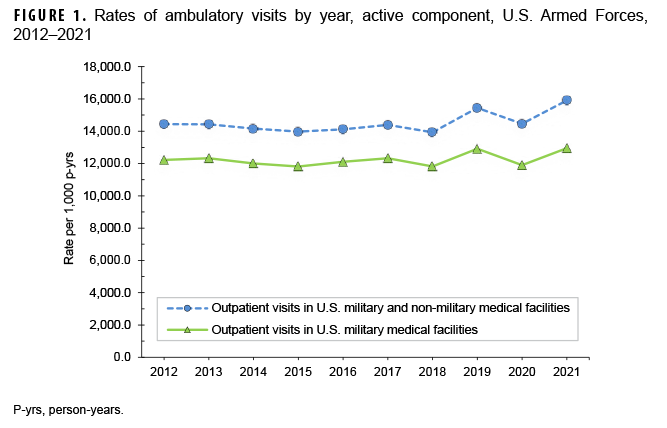
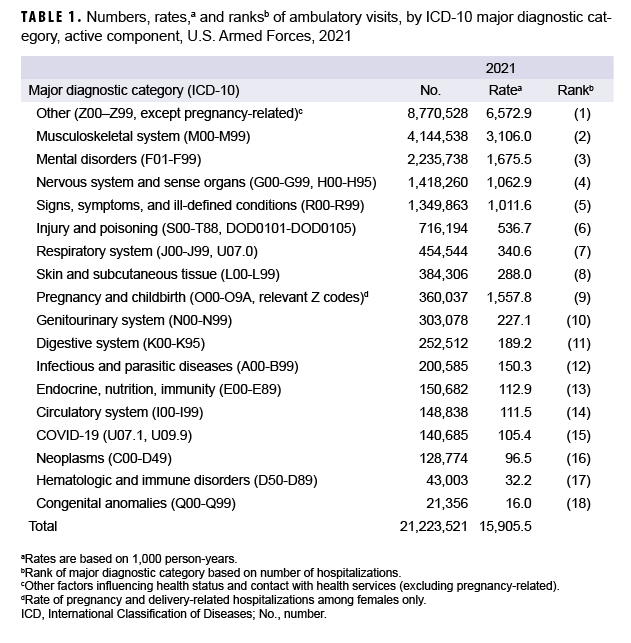
During 2021, there were 21,223,521 ambulatory visits of active component service members. “Visits” refers to encounters accomplished via in-person clinical meetings as well as “telehealth” encounters. The crude annual rate (all causes) was 15,905.5 visits per 1,000 person-years (p-yrs) or 15.9 visits per p-yr; thus, the average number of ambulatory encounters during the year was nearly 16 encounters per service member (Table 1). The crude annual rate for 2021 was the highest of the period 2012–2021 (Figure 1). The rate of documented ambulatory visits in U.S. military and non-military medical facilities in 2021 was 13.8% higher than the lowest rate in the interval 2012–2020 (13,978.5 per 1,000 p-yrs in 2015) and 1.2% higher than the previous peak in 2019 (15,718.5 visits per 1,000 p-yrs) (Figure 1, data not shown). In 2021, 41.3% of ambulatory visits were classified into the “other” category (i.e., other factors influencing health status and contact with health services, excluding pregnancy-related), which includes health care not related to a current illness or injury (Table 1). Such care includes routine and special medical examinations (e.g., periodic, occupational, or retirement), therapeutic and rehabilitative treatments for previously diagnosed illnesses or injuries (e.g., physical therapy), immunizations, counseling, deployment-related health assessments, and screening.
In 2021, there were 12,452,993 documented ambulatory visits for illnesses and injuries (ICD-10: A00–T88, including relevant pregnancy Z-codes; U07.0, U70.1, and U09.9), not including diagnoses classified as “other,” for a crude annual rate of illnessand injury-related visits of approximately 9.3 visits per p-yr (data not shown). During the prior 9 years, the crude annual rate of ambulatory visits for illnesses and injuries in 2021 was exceeded only by the rate in 2016 (9.6 visits per year).
Ambulatory visits, by diagnostic categories
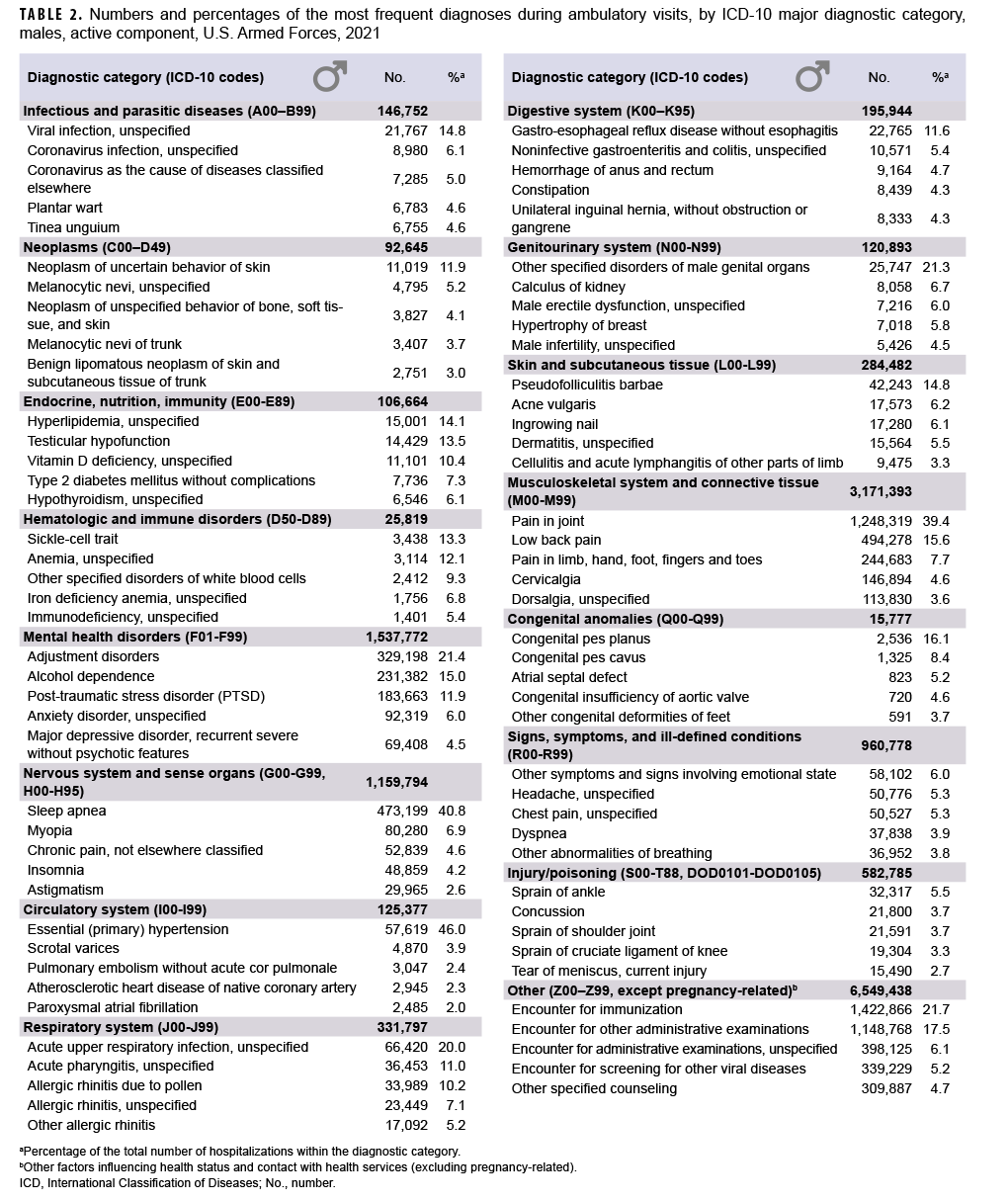
In 2021, 4 major diagnostic categories accounted for almost three-quarters (73.5%) of all illness- and injury-related ambulatory visits among active component service members (not including diagnoses classified as “other”): musculoskeletal system/connective tissue disorders (33.3%); mental health disorders (18.0%); disorders of the nervous system and sense organs (11.4%); and signs, symptoms, and ill-defined conditions (10.8%) (Table 1). COVID-19 accounted for 0.66% of the total ambulatory visits in 2021, an increase from 2020 when COVID-19 was associated with just 0.44% of all visits. Among visits for illness and injury, COVID-19 encounters represented 1.1% of visits in 2021 and 0.74% of visits in 2020.
During 2021, the annual rates of visits in 5 major diagnostic categories of illness and injury were the highest for any year in the 10-year period of 2012–2021 (Table 1; data not shown). These peak rates were recorded for the categories of mental health disorders; nervous system and sense organs; signs, symptoms, and ill-defined conditions; genitourinary system; and hematologic disorders. The category for COVID-19 was added to the categories of illness and injury for last year’s report.2 The number of visits and rates for COVID-19 increased from 83,405 and 62.9 per 1,000 p-yrs in 2020 to 140,685 and 105.43 per 1,000 p-yrs in 2021. Of the remaining 11 major diagnostic categories of disease and injury, 7 categories had higher rates in 2021 than were recorded in the years 2019 and 2020. There were 4 diagnostic categories of illness and injury for which the 2021 rates were notably lower than the annual rates for most of the 10-year period. Specifically, the 2021 rate for musculoskeletal disorders (3,106.0 per 1,000 p-yrs) was only the fifth highest of the period. More distinctively, the 2021 rates for infectious and parasitic diseases (150.3 per 1,000 p-yrs), injury and poisoning (536.7 per 1,000 p-yrs), and respiratory system disorders (340.6 per 1,000 p-yrs) ranked 8th, 9th, and 10th among rates observed for those categories during the 10-year period.
In general, the relative distributions of ambulatory visits by ICD-10 diagnostic categories remained stable over the surveillance period (Table 1). In a comparison of the numbers and rates of visits attributable to each of the 17 major diagnostic categories (excluding COVID-19) in the years of interest 2015–2021, the rank orders of the most numerous categories remained relatively stable. The rank orders of the 5 least numerous of the diagnostic categories tended to vary from year to year. COVID-19 ranked 16th and 15th in total visits during 2020 and 2021, respectively.
Ambulatory visits, by sex
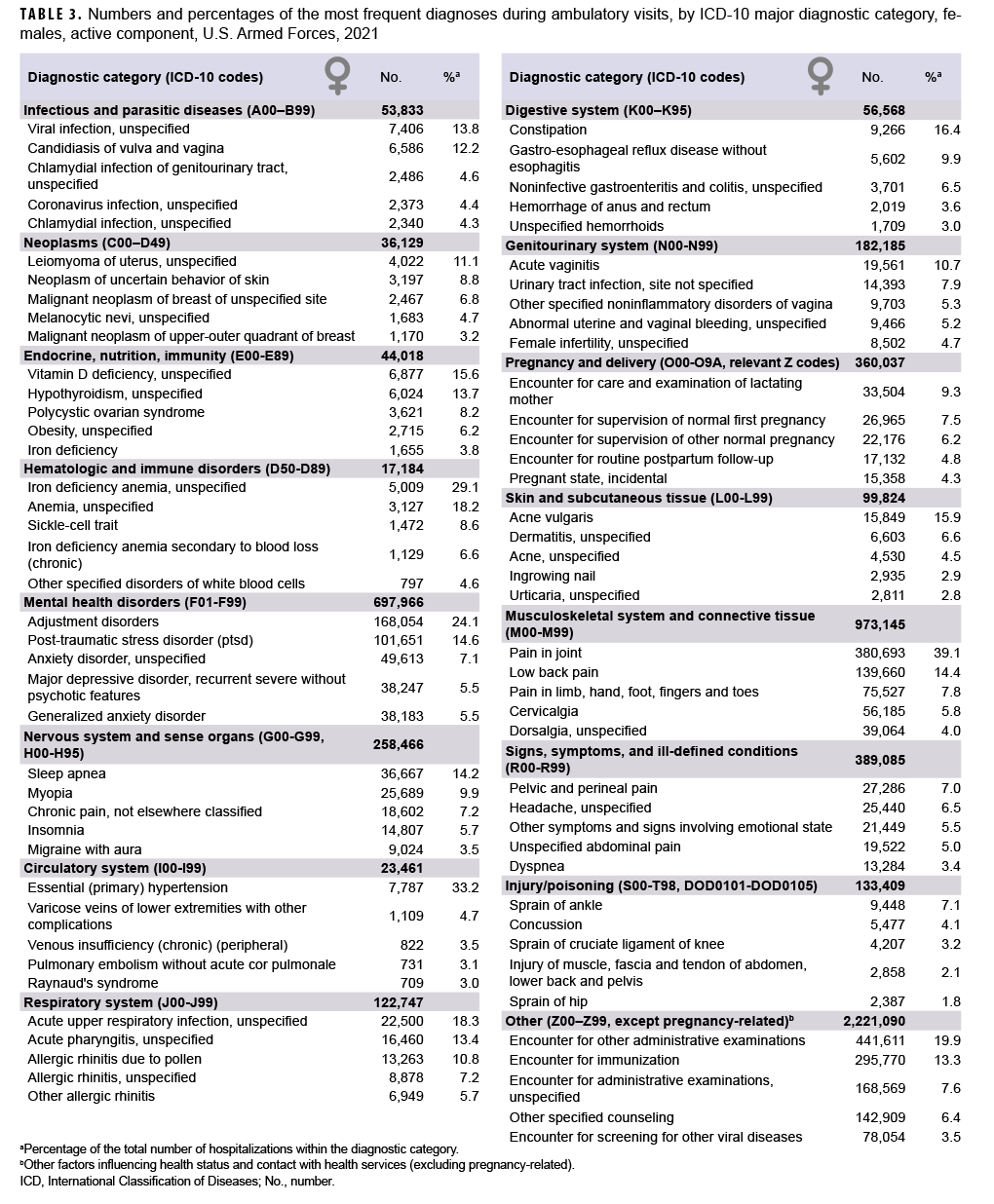
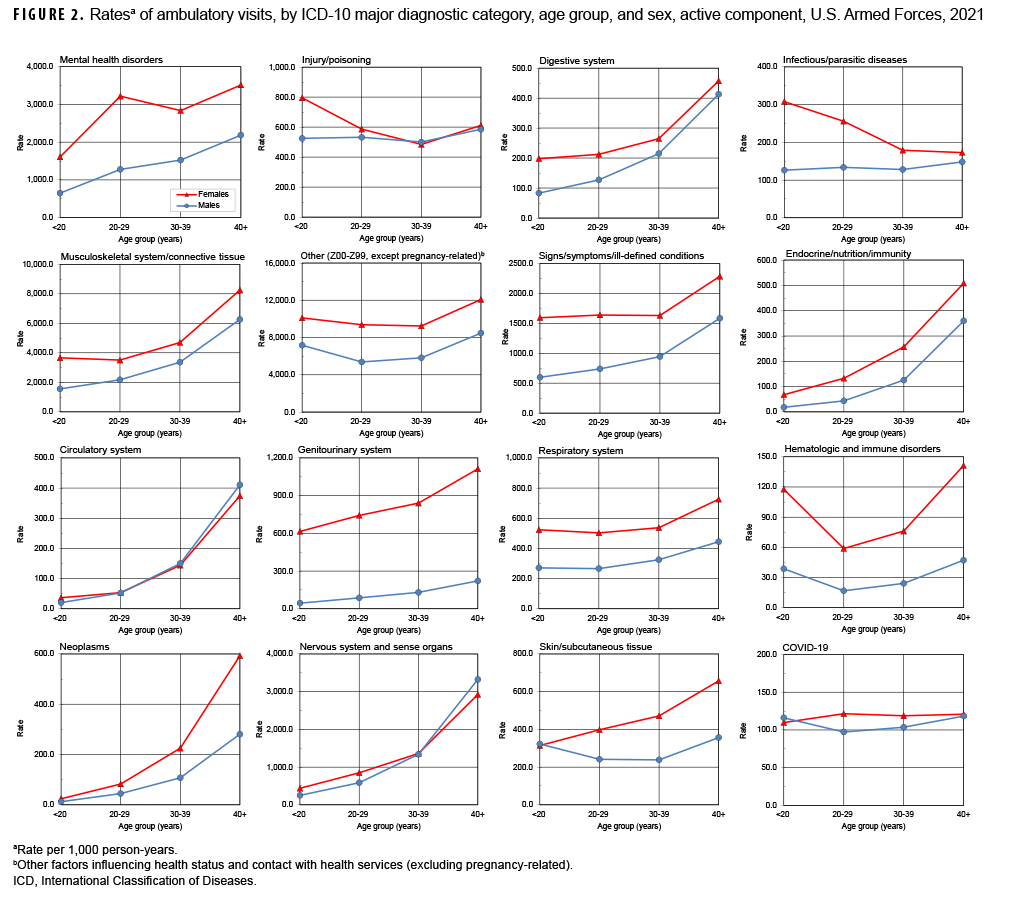
In 2021, male service members accounted for nearly three-fourths (72.0%) of all illness- and injury-related visits; however, the annual crude rate among female service members (15.1 visits per p-yr) was 85.2% higher than that among males (8.1 visits per p-yr) (data not shown). Excluding pregnancy- and delivery-related visits (which accounted for 10.3% of all non-Z-coded ambulatory visits among female service members), the illness and injury ambulatory visit rate among female service members was 13.5 visits per p-yr. As in the past, rates for illness- and injuryrelated categories were generally higher among female than male service members (Figure 2).
Among all illness- and injury-specific diagnoses, 4 of the 5 diagnoses with the largest numbers of ambulatory visits were the same for male and female service members (Tables 2, 3). However, the crude rate (per 1,000 p-yrs) was at least 35% higher among female than male service members for each of these 4 common diagnoses: pain in joint (female: 1,647.1; male: 1,131.5; female:male rate ratio [RR]: 1.46); low back pain (female: 604.3; male: 448.0; RR: 1.35); adjustment disorders (female: 727.13; male: 329.2; RR: 2.44); and pain in the limb, hand, foot, fingers, and toes (female: 326.8; male: 221.8; RR: 1.47) (data not shown). Four other diagnoses were among the 10 most common diagnoses for both male and female service members: post-traumatic stress disorder (PTSD); cervicalgia; dorsalgia; and anxiety disorder, unspecified. Of note, among male service members, sleep apnea was the 3rd most frequent illness- or injury-specific primary diagnosis during ambulatory visits and alcohol dependence was ranked 6th, but neither of these diagnostic categories ranked among the 10 most common diagnoses among female service members. Among female service members, the 9th and 10th most common diagnoses were major depressive disorder, recurrent, severe without psychotic features, and generalized anxiety disorder, but neither was among the 10 most common diagnoses among male service members (Tables 2, 3).
Across diagnostic categories, relationships between age group and ambulatory visit rates were broadly similar among male and female service members (Figure 2). For example, among both sexes, ambulatory visit rates for neoplasms and circulatory disorders among those aged 40 years or older were 10 or more times the rates among those younger than 20 years old; in contrast, clinic visit rates for infectious and parasitic diseases were lower among the oldest compared to the youngest service members. As in the past, ambulatory visit rates for disorders of the nervous system; digestive system; endocrine system, nutrition, and immunity; and musculoskeletal system/connective tissue rose more steeply with advancing age than most other categories of illness or injury (for which rates were relatively stable or only modestly increased) (Figure 2). Ambulatory visit rates for diagnoses of COVID-19 infections were relatively stable with advancing age.
Dispositions after ambulatory visits
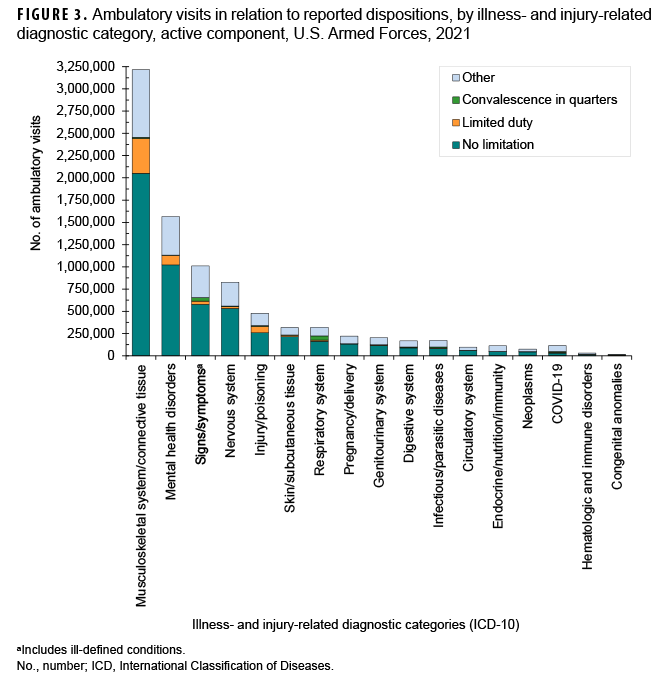
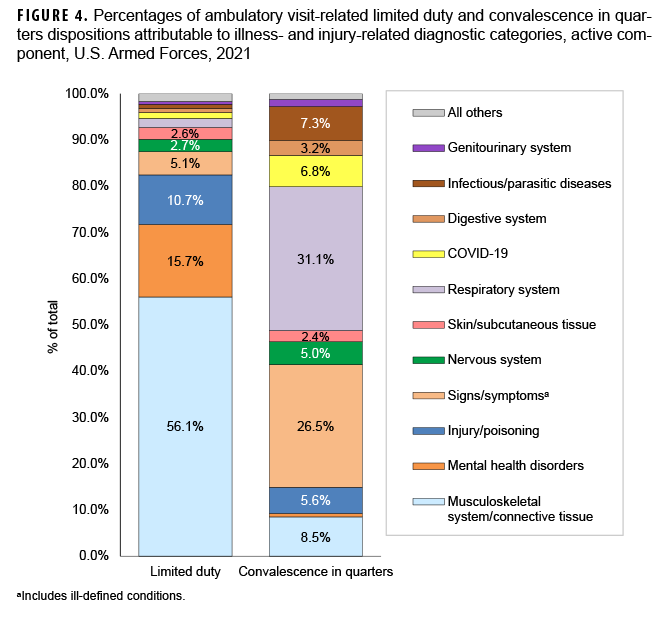
Because disposition codes are assigned to ambulatory medical encounters that occur only at military treatment facilities (MTFs), the following metrics do not include outsourced care. Approximately 60.9% of all illness- and injury-related visits resulted in “no limitation” (i.e., duty without limitations) dispositions (data not shown). Of illness- and injury-related visits, 1.6% resulted in “convalescence in quarters” dispositions (data not shown). The illness- and injury-related diagnostic categories with the highest proportions of “limited duty” dispositions were injuries and poisonings (15.5%) and musculoskeletal system/connective tissue disorders (12.3%) (Figure 3). The illness- and injury-related diagnostic categories with the highest proportions of “convalescence in quarters” were infectious and parasitic diseases (6.2%) and diseases of the respiratory system (14.2%). Musculoskeletal system/connective tissue disorders (56.1%) accounted for more than one-half of all “limited duty” dispositions, and mental health disorders (15.7%) and injury/poisoning (10.7%) together accounted for more than one-quarter (26.4%) (Figure 4). Diseases of the respiratory system accounted for nearly one-third (31.1%) of all “convalescence in quarters” dispositions—more than twice as many (n=45,347) as any other diagnostic category, except signs and symptoms (26.5%).
Ambulatory visits accomplished via telehealth
In the years 2016 and 2018 the percentages of ambulatory encounters that were associated with telehealth encounters approximated 14% (data not shown). In 2020, the first year of the COVID-19 pandemic, the percentage of encounters that were attributed to telehealth was 19.2% (data not shown). The number of telehealth encounters had increased by 942,859 encounters between 2018 and 2020, but the number of non-telehealth encounters fell by 964,119 during that interval (data not shown). In the second year (2021) of the pandemic, the total number of outpatient encounters was 21,223,521, a much larger total than was recorded in 2020 (19,070,128). In 2021, 14.8% of outpatient encounters were accomplished via telehealth, a noteworthy decrease from 2020 (data not shown). Of the 18 different major diagnostic categories (including the new category for COVID-19), only 9 of the categories had 10% or more of their encounters via telehealth. The leading percentages of telehealth visits were for COVID-19 (40%); endocrine/nutrition/immunity (30%); “other” (27%); infectious and parasitic diseases (23%); hematologic and immune disorders (21%); neoplasms and genitourinary system disorders (both 12%); and disorders of the circulatory system and signs, symptoms, and ill-defined conditions (both 10%) (data not shown). These 9 categories accounted for 85.5% of all ambulatory encounters accomplished via telehealth.
Editorial Comment
During 2019–2021, the numbers of illness- and injury-related ambulatory visits in relation to their reported primary causes decreased in 2020 and then increased significantly in 2021. In 2021, musculoskeletal system/connective tissue and mental health disorders accounted for more than one-half (51.3%) of all illness- and injury-related diagnoses documented on standardized records of ambulatory encounters. Over the course of the 3-year period that included 1 year before, and 2 years after, the onset of the COVID-19 pandemic (2019–2021), the incidence rates of 5 major illness- and injury-related categories (mental disorders; nervous system and sense organs; signs/symptoms and ill-defined conditions; disorders of the genitourinary system; and hematologic and immune disorders) increased to peak numbers of ambulatory visits and rates in 2021; 3 illness- and injury-related categories showed consistent decreases.
One factor that partially explained the observed decreases in ambulatory encounters in 2020 is the COVID-19 pandemic which directly affected the health of many service members whether or not they acquired a coronavirus infection. During 2020, indirect effects of the pandemic could be attributed to the implementation of preventive measures taken to lessen transmission of the virus. Such measures included restrictions on housing, training, and social gatherings, all of which may have reduced the incidence of injuries and illnesses in the service member population. The reduced incidence would be reflected in the counts of ambulatory visits in the MHS. In addition, during 2020, medical facilities were encouraged to increase the use of telehealth procedures in order to reduce the risks of virus transmission in the health care settings. These telehealth initiatives may have succeeded in reducing the incidence of not only SARS-CoV-2 infections but also other infectious diseases.
The second year of the pandemic, 2021, was marked by the introduction of efficacious COVID-19 vaccines. Although the vaccines over time undoubtedly reduced the incidence of COVID-19 disease below its potential peak levels, the emergence of variant strains of the virus and the careful surveillance for SARS-CoV-2 infections resulted in an increase in cases detected despite the extensive control measures. The fact that incidence rates of the more common categories of illness and injury rose in 2021 to exceed pre-pandemic levels may reflect several factors, including the postponement of care for some common conditions during 2020, the increased ability of health care facilities and staff to accommodate patients with precautionary measures during 2021, and the increased incidence of some diagnoses (e.g., mental health disorders) as a result of the social impact of pandemic measures. The fact that the 2021 rates of visits for infectious and parasitic diseases, injury and poisoning, and respiratory system disorders declined while the rates for most other disease and injury categories increased suggests that steps taken to reduce spread of SARS-CoV-2 had a positive effect on those disorders.
Several limitations should be considered when interpreting the findings of this report. For example, ambulatory care that is delivered by unit medics and at deployed medical treatment facilities (such as in Afghanistan or Iraq or at sea) have not been included. In turn, this summary does not reflect the experience of active component military members overall to the extent that the natures and rates of illnesses and injuries may vary between those who are deployed and those who are not deployed.
In addition, this summary is based on primary (first-listed) diagnosis codes reported on ambulatory visit records. As a result, the current summary discounts morbidity related to comorbid and complicating conditions that may have been documented in secondary diagnostic positions of the healthcare records. Furthermore, the accuracy of reported diagnoses likely varies across conditions, care providers, treatment facilities, and clinical settings. Although some specific diagnoses made during individual encounters may not be definitive, final, or even correct, summaries of the frequencies, natures, and trends of ambulatory encounters among active component members are informative and potentially useful. For example, the relatively large numbers of ambulatory visits for mental health disorders in general and the large numbers of visits for organic sleep disorders among males, reflect patterns of responses by the MHS to the effects of combat- and deployment-related stresses on active component service members.
Also, this report documents all ambulatory healthcare visits but does not provide estimates of the incidence rates of the diagnoses described. In contrast to common, self-limited, and minor illnesses and injuries that require very little, if any, follow-up or continuing care, illnesses and injuries that necessitate multiple ambulatory visits for evaluation, treatment, and rehabilitation are overrepresented in this summary of the ambulatory burden of health care. Finally, medical data from sites that were using the new electronic health record for the Military Health System, MHS GENESIS, between July 2017 and October 2019 were not available in the DMSS at the time of the analysis. These sites include Naval Hospital Oak Harbor, Naval Hospital Bremerton, Air Force Medical Services Fairchild, and Madigan Army Medical Center. Therefore, medical encounter data for individuals seeking care at any of these facilities from July 2017 through October 2019 were not included in the current analysis.
References
- Armed Forces Health Surveillance Branch. Ambulatory visits, active component, U.S. Armed Forces, 2016. MSMR. 2017;24(4):16–22.
- Armed Forces Health Surveillance Division. Ambulatory visits, active component, U.S. Armed Forces, 2020. MSMR, 2021;28(5):18–25.