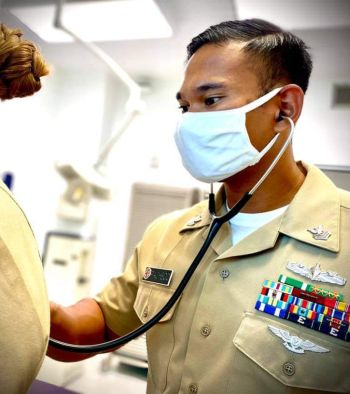
 Hospital Corpsman 1st Class Aris Pacheco listens to a patient’s lungs during a routine exam at the Naval Hospital Guantanamo Bay’s Primary Care Clinic. More than 100 staff members at Naval Medical Readiness Training Command Guantanamo Bay were recognized during the awards ceremony. (Photo by Seaman Lauren Nguyen.)
Hospital Corpsman 1st Class Aris Pacheco listens to a patient’s lungs during a routine exam at the Naval Hospital Guantanamo Bay’s Primary Care Clinic. More than 100 staff members at Naval Medical Readiness Training Command Guantanamo Bay were recognized during the awards ceremony. (Photo by Seaman Lauren Nguyen.)
“From the men and women who work tirelessly to clean our facilities to the pharmacy staff, emergency departments, public health teams, laboratory staff, corpsmen, medics, nurses, and physicians, this year has really been a trying time,” Alvarado said. “It’s fitting that we come together today to recognize a few of you.”
His observations were echoed by Dr. Paul Cordts, DHA’s chief medical officer and deputy assistant director for medical affairs.
“We see the innovation here (at DHA) that’s coming from you…we’re now on our sixth iteration of our practice management guidelines,” Cordts said. “As a leader you need to think of the resilience of your team and what it will take to keep them going and doing their heroic work.”
The awards display military medicine’s vast capabilities, especially during an unexpectedly adverse and potentially deadly situation. According to Heidi King, DHA patient safety program manager for medical affairs, it’s situations like these that show military training and resourcefulness, as well as teamwork, and can bring stability to chaos.
“There have been so many awesome stories that have come in that are being recognized, both individuals and teams, to safeguard our staff as well as our patients, and this just shows how we are ready and reliable and resilient during this heightened stress and uncertain times,” King said.
One example, featuring dozens of awardees, was Naval Hospital Rota in Spain.
Like other commands outside the continental United States, proactive and creative responses including a “pseudo-ICU” were needed early in the pandemic to deal with factors such as the lack of established evidence-based practices or higher authority guidance due to COVID-19’s swift spread through Europe prior to its arrival in the United States.
“Battling COVID and social isolation, the team at Naval Hospital Rota was able to effectively mitigate spread and yield 100% force health protection success as evidenced by Naval Hospital Rota’s selection for this and other awards,” said Navy Cmdr. David Paz, Rota’s chief medical officer.
The Carl R. Darnall Army Medical Center in Ft. Hood, Texas, also recognized dozens of staff members who quickly adapted to their new reality.
“The biggest contributors were open communication, team collaboration, and knowledge-sharing, as well as encouragement and massive cross-training,” said Sonya Woodson, chief of patient safety at Ft. Hood. “It was instrumental in the team’s ability to not only overcome challenges, but create multiple avenues to delivering health care innovations.”
Another example was Naval Hospital Guantanamo Bay in Cuba, where more than 100 staff members were recognized.
“The COVID-19 pandemic has placed a spotlight, of course, on our health care heroes,” said Executive Officer Navy Capt. Anja Dabelić. “Through teamwork, resiliency and championing, Naval Hospital Guantanamo Bay staff has adapted to these challenges through multi-disciplinary teams and a COVID-19 task force.”
Measures taken at Naval Hospital Guantanamo Bay included the construction of a triage center, quarantine tent, a negative pressure isolation center, single points of entry for patients and staff and a drive-through pharmacy.
“This is truly a peer-to-peer award, and you all spent a lot of time putting in the effort to recognize your peers at the front line of what military medicine is all about,” said Dr. Brian Lein, DHA assistant director for health care administration, “patient safety, focusing on the patient, and going that extra mile in support of staff that are around you.”
The DHA Patient Safety Program is accepting and reviewing submissions for the next round of awards. Military hospitals and clinics can nominate as many individuals and teams as they wish.
Anyone with questions about the award can email the Patient Safety Program. To nominate an individual or team, please visit the Click to closeTeamSTEPPSTeam Strategies and Tools to Enhance Performance and Patient Safety (TeamSTEPPS) is an evidence-based teamwork system designed to improve the quality, safety and efficiency of healthcare. TeamSTEPPS consists of a collection of instructions, materials and tools to help drive a successful teamwork initiative from the initial planning to implementation through to sustainment. The system is designed to improve patient safety using a three-phase approach: Phase I Assessment: Facility determines organizational readiness; Phase II Planning, Training & Implementation: Facility “decides what to do” and “makes it happen;” and Phase III Sustainment: Facility spreads the improvements in teamwork performance, clinical processes and outcomes resulting from the TeamSTEPPS initiative.TeamSTEPPS page on the Patient Safety Learning Center site.